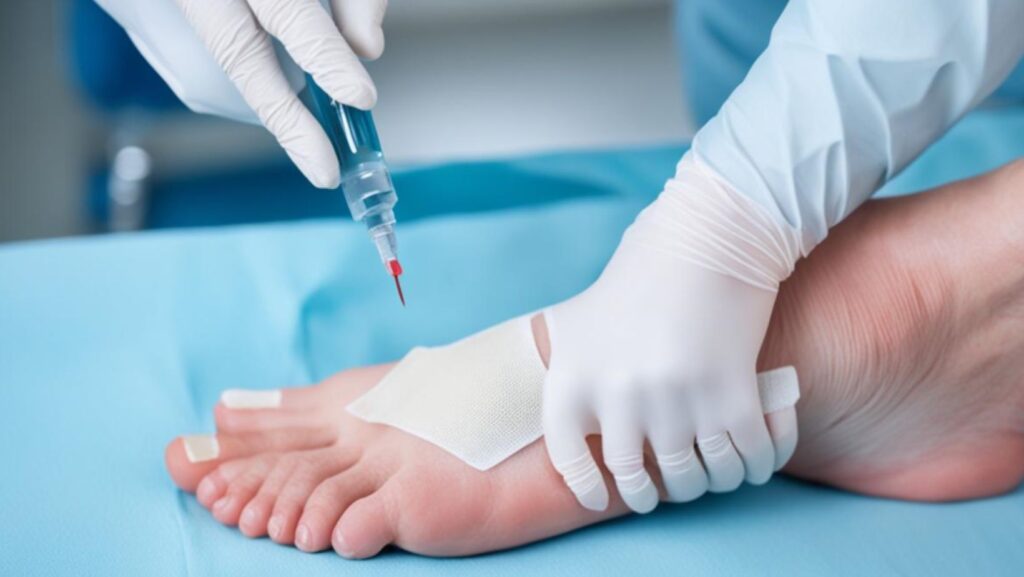
Diabetic wounds often heal slowly. This happens because diabetes affects the body in many ways. High blood sugar, poor blood flow, nerve problems, and weak immunity can all slow wound healing. Despite these challenges, diabetic wounds can be managed well with the right care.
This article looks at why diabetes makes wounds heal slowly. It also gives advice on how to spot and treat diabetic wounds. Plus, it covers the kinds of dressings used in diabetic wound care.
Why Diabetes Causes Slow-Healing Wounds
Diabetes slows down the body’s wound healing. It affects many things, like high blood sugar, bad circulation, nerve issues, and a weak immune system.
High Blood Glucose from Diabetes
Diabetes slows healing because it raises blood sugar levels. This harms blood vessels and nerves, causing poor blood flow and less feeling in the body’s parts. Wounds find it tough to get what they need to heal right.
About 37.3 million people in the US have diabetes, which is 11.3% of the population. It’s vital to keep blood sugar levels normal to help wounds heal faster.
Poor Circulation from Diabetes
Diabetes can lead to poor blood flow, which makes it hard for wounds to get oxygen and nutrients. It happens because diabetes damages blood vessels, causing a condition called peripheral vascular disease. People with diabetes are twice as likely to develop peripheral vascular disease.
Almost half of people with peripheral artery disease also have diabetes. This shows how closely diabetes and circulatory issues are linked in healing wounds.
Diabetic Neuropathy
Diabetes often causes diabetic neuropathy, which slows healing too. It affects the nerves in the hands and feet. About 60% of diabetes patients get neuropathy, which can lower sensation. This makes it hard to notice injuries or slow-healing wounds.
Weakened Immune System from Diabetes
Diabetes weakens the immune system. This makes it harder to fight infections that can slow down healing. High blood sugar levels help bacteria thrive, making it harder for the body to fight infections.
People with diabetes often get foot ulcers if they don’t manage their wounds properly. Approximately 20-25% of diabetes patients will get foot ulcers at some point.
Diabetes affects wound healing in several ways. High blood sugar, circulation problems, nerve damage, and a weak immune system play a big role. Managing diabetes well is key to avoiding these issues and healing wounds better.
Identifying and Treating Diabetic Wounds
It’s vital to spot a diabetic wound that isn’t healing right to act quickly. Look for ongoing swelling or signs of infection. If a wound doesn’t heal after four weeks, this could mean trouble.
If you have a wound that won’t heal, get medical help fast. Diabetic people should closely follow their doctor’s advice. They might need special dressings like foam, alginate, or hydrogel.
Signs a Diabetic Wound Isn’t Healing Properly
- Persistent inflammation
- Signs of infection (e.g., redness, swelling, warmth, pus)
- A wound that takes longer than four weeks to heal
Tips to Help a Diabetic Wound Heal Faster
- Treat cuts and scrapes immediately
- Keep the wound clean and covered

- Avoid putting pressure on the wound
- Work closely with a healthcare provider to develop the best treatment plan
Common Dressings for Diabetic Wound Care
|
Dressing Type |
Description |
|
Foam Dressings |
Absorb exudate and provide a moist wound environment |
|
Alginate Dressings |
Absorb high levels of exudate and help maintain a moist wound bed |
|
Hydrogel Dressings |
Provide a moist wound environment and help rehydrate the wound bed |
Conclusion
Diabetes can slow down the wound-healing process, making it harder to treat wounds. But, with the right care, diabetic wounds can get better. Things like high blood sugar, bad circulation, nerve damage, and a weak immune system make healing slow. It’s important to watch for signs that a wound isn’t healing and to get help managing it from a healthcare provider.
Taking a full approach to diabetic wound care is key for foot health. This approach includes getting insights from research to find out how common these wounds are. It also focuses on catching problems early and using treatments that work. This can help diabetic people heal their wounds better and lower the risk of more trouble.
Overall, a plan that fits a person’s specific needs, along with always learning and getting support, can improve wound healing. By putting diabetic wound care first, healthcare teams and diabetic people can team up to do better. This helps gain good foot health and healing from wounds.
FAQ
What are the Key Factors That Contribute to Slow Healing of Diabetic Wounds?
High blood sugar, poor blood flow, nerve damage, and weak immunity slow down wound healing in diabetics.
How can I Recognize if a Diabetic Wound is Not Healing Properly?
If you see the wound stays inflamed, gets infected, or doesn’t heal in four weeks, it may be bad. Get quick medical help, then.
What can I do to Help a Diabetic Wound Heal Faster?
To speed up healing, treat any cuts right away. Keep them clean, covered, and avoid pressure. Also, working with a doctor for the right dressings helps a lot.
What are Some Common Dressings used in Diabetic Wound Care?
Doctors often use foam, alginate, and hydrogel dressings for diabetic wounds. These dressings support quick healing and cut down on problems.
Why is it Important to Have a Comprehensive Approach to Diabetic Wound Care?
A broad approach to wound care is key for good foot and overall health. It’s especially important for managing diabetes’ effects on healing. The right care helps wounds heal faster and avoids big issues like foot ulcers.